Credentialing
A faster route to enrollment. Streamline the credentialing process and prevent lags in payment due to un-earned or expired credentials. Utilize our intuitive Pulse portal coupled with expert-supported service that provides an end-to-end solution for your organization’s credentialing needs. Our guided workflow can help you gain compliance quickly, saving you valuable time and allowing you to earn reimbursements for your services as soon as possible.
With our services, you can:
- Easily manage documents in one location
- Eliminate redundancies in data gathering
- Ensure compliance with all payer regulations
Reduce
credentialing
times by up to
50%

“A devoted team that can take time-consuming tasks off my plate and complete the credentialing process quickly? That’s exactly why we needed TPS! ”
– Michelle Buchan, North Medical Billing
Highlighted Resources
Streamline the credentialing process and prevent lags in payment due to un-earned or expired credentials.
Discover how Vascular Surgery Associates’ credentialing and re-credentialing needs were completed in 90 days, well under the industry average.
Learn how North Medical Billing saved approximately 20 hours a week with TriZetto Provider Solutions’ credentialing services.
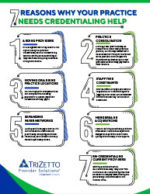
Are you prepared for enrollment? Our infographic can help you identify if you need credentialing help.
New to the credentialing process? Download our whitepaper and read about the steps needed to streamline your credentialing.